How can we end the health disparity that exists in asthma care?
ALLERGY – a damaging immune reaction to a usually innocuous (harmless) and ubiquitous (found everywhere) substance
ASTHMA – narrowing of airways that causes wheezing, often in response to an allergic reaction
IMMUNOLOGY – the study of the immune system and how the body protects itself from infectious diseases
SOCIO-ECONOMIC – based on social and economic factors (such as social class, education or income)
PALYNOLOGY – the study of pollen grains and other spores
PLASMA CELL – a white blood cell, called a B cell, that is capable of producing and secreting antibodies
CYTOKINES – proteins which affect the communication between other cells
T HELPER CELL – a white blood cell that aids the activity of the immune system by releasing cytokines (for example, the cytokine IL4 can cause B cells to release allergic antibodies)
ANIMAL MODEL – an animal used in medical/scientific research
Answering these questions could help millions of people around the world to control and manage this condition. Based at Edward Waters University (EWU), Dr Brian Seymour, a professor of biology with an earned doctorate in immunology, has spent many years studying the body’s immune response to asthma to unravel the mechanism of this disease. He is also investigating why certain socio-economic groups are more likely to be afflicted by this disease than others. He is leading valuable community outreach effort to improve health literacy as a strategy to reduce disparities in health care.
A CAREER IN IMMUNOLOGY
Working at a blood bank after graduating from Southern Illinois University with a bachelor’s degree in biology, the future Professor Seymour became fascinated by the way a recipient’s body could reject a donor’s blood after multiple transfusions, even if they were a match in terms of red blood cell type. This was due to discrepancies in white blood cell type, as was observed from his laboratory test. His work in blood testing led to a position working with kidney donors, testing for compatibility between donor and recipient. The role of the immune system in recognising the body’s own cells versus foreign ones sparked Professor Seymour’s interest and was the catalyst that motivated him to pursue graduate studies in immunology. Having achieved his master’s in clinical science with a major in clinical immunology, he embarked on a career in research studying the immune responses to allergens.
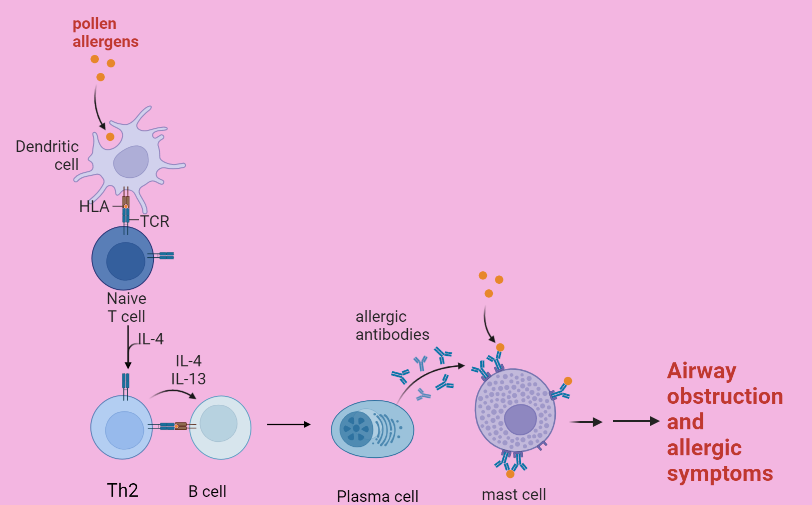
While working at the DNAX Research Institute, Professor Seymour researched the proteins (cytokines) that are released by T helper type 2 (Th2) cells, a type of white blood cell which is active in the immune system’s harmful response to allergens. By blocking cytokine release, the team found it could limit the amounts of antibodies produced by plasma cells (antibody-producing white blood cells) that are elevated during the body’s allergic asthma response. Professor Seymour says, “As we were using animal models of lung inflammation, we were, indeed, unravelling the mechanism of allergic asthma.”
ANIMAL MODELS
Professor Seymour received funding from the Tobacco-Related Disease Research Program (TRDRP) in California and the DNAX Research Institute to pursue a PhD in Immunology at the University of California, Davis (UCD). There, he studied the effects of second-hand cigarette smoke, also known as environmental tobacco smoke (ETS), on the immune system. Prior to his research, epidemiological studies had suggested that ETS was responsible for increases in cancer and asthma rates. He acknowledges this was difficult to prove, due to “many environmental pollutants that one is exposed to on a daily basis, such as diesel exhaust particles”. He was part of an interdisciplinary team which used animal models (specifically mice) to study the effect of ETS on allergic asthma, without external environmental pollutants. Some mice were kept as control subjects, while others were exposed to ETS. They were all also exposed to allergens that are known to cause allergic asthma. All of the mice were then examined for three parameters that are characteristic of allergic asthma: Th2 cytokines, allergic antibodies and bronchial hyperresponsiveness (wheezing). Professor Seymour explains, “These three parameters were significantly enhanced in the groups exposed to ETS when compared to the control groups that were not exposed to ETS.”
This was the first study using mice in a controlled environment to prove that ETS had a harmful effect on allergic asthma. This research, along with similar work from others, led to the ban on smoking in public areas in California.
ENVIRONMENTAL FACTORS
EWU, where Professor Seymour lectures and conducts research, is in an area referred to by public health officials as Health Zone 1 of the six health zones in Duval County, Jacksonville. This area has a high population density and is mostly urban landscape. It is ranked number one for asthma-related hospitalisations (including emergency room visits) and its asthma-related death rate is above the average in Florida. This area is also the least economically advantaged in Duval County; its population is the poorest and least educated. Professor Seymour explains, “Health disparity is not only closely linked to social or economic disadvantage but also to exposure to environmental factors.” He believes that economic, social and environmental factors are all interconnected.
ASTHMA IN THE AFRICAN AMERICAN COMMUNITY
With a focus on socio-economic factors, Professor Seymour’s team wanted to assess the connection between high levels of allergic asthma in the African American population around Jacksonville, specifically in Health Zone 1. Professor Seymour explains, “In the US, morbidity and mortality from allergic asthma is highest in the African American population.” The team collected blood samples from random residents of Health Zone 1 during the pollen season and found that 64% of participants had elevated levels of allergic antibodies. The researchers then studied the concentration of pollen grains in the air in Health Zone 1, using a monitor on the roof of EWU. “We found pollen grains were elevated to levels deemed as severe by the National Allergy Bureau (NAB),” says Professor Seymour. This finding led the team to speculate that high levels of pollen grains may be partly responsible for high rates of allergic symptoms in this area.
AIMING FOR HEALTH EQUITY
Professor Seymour acknowledges that there is still a long way to go before health equity is attained in the US. He says, “A vulnerable community will have poor health outcomes due to the health disparities that exist in that environment.” Issues include access to affordable health care, access to healthy food and lack of public health facilities in particular communities. These factors lead to a situation where, according to Professor Seymour, “ethnic minority groups and the vulnerable populations are disproportionately burdened by many diseases”. Researchers like Professor Seymour are working diligently to bring awareness and to provide substantive empirical evidence that policy makers will need to address the health disparity that exists in Health Zone 1.
 DR BRIAN SEYMOUR
DR BRIAN SEYMOURProfessor of Biology and Research Director of the Center for the Prevention of Health Disparities, Edward Waters University, Jacksonville, Florida, USA
FIELDS OF RESEARCH: Immunology, Palynology
RESEARCH PROJECT: Studying the airborne pollen in Northeast Florida and how it correlates to the high rate of allergic asthma in Health Zone 1, a vulnerable community in urban Jacksonville
FUNDER: US National Science Foundation (NSF)
Grant ID: 2000433
WHAT IS IMMUNOLOGY AND WHY CHOOSE IT AS A CAREER?
Immunology is the study of the immune system and how life forms fight infectious diseases. Immunologists can be lab-based (conducting research) and clinical (working directly with patients in a medical setting), studying a wide range of diseases such as allergies, immunodeficiency, neurodegenerative conditions (e.g. Alzheimer’s) and cancer. The discipline also covers both academia and industry. Vaccine development is another area of research in immunology. The British researcher Edward Jenner, whose work in the late 18th century led to developing the vaccine against smallpox, is often credited for immunology becoming a science. Vaccination is likely responsible for saving more lives than any other aspect of medicine.
In studying immunology, it is impossible to ignore the importance of public health and the social and environmental factors which have an influence upon different socio-economic groups and their respective health. Professor Seymour states, “Health disparities still exist, and we are far from attaining health equity in the US.” To understand immunological problems and achieve health equity, it is important to consider many factors. Research in immunology may impact upon legislation, to protect people’s health. For example, Professor Seymour’s work played a role in smoking being banned in public places in California.
Reference
https://doi.org/10.33424/FUTURUM288
Professor Seymour finds positives in both lines of work. He says, “Ultimately, both industry and academia have the goal of making life better for humanity.” While industry offers more financial resources for targeted research and development, researchers in this area are more constrained by the demands of the industry in which they are working. Academia gives greater flexibility for researchers to write their own proposals and offers teaching opportunities to work with students from a range of backgrounds, which for Professor Seymour, “is a satisfaction that goes beyond the financial gains”.
RESEARCH OPPORTUNITIES
New fields of immunology are constantly being developed. One such field is personalised (or precision) medicine. This involves targeted therapy for a specific problem. For example, a physician can treat a patient for a specific pollen allergy by training a patient’s immune system to become unresponsive to the particular pollen. Computational skills will be particularly important in the future. Professor Seymour explains, “The next generation of immunologists will need to know bioinformatics, while being knowledgeable in the field of immunology in order to unravel big data to understand data trends.”
WORKING WITH COMMUNITIES
The Center for the Prevention of Health Disparities is involved with multiple public outreach programmes. Professor Seymour is a board member of the Northeast Florida Health Education Center. This centre, in collaboration with EWU, offers tobacco cessation classes in Health Zone 1 of Duval County, Florida, to assist residents of the community to quit smoking. EWU also organises internships and postbaccalaureate programmes for students. Professor Seymour is also the lead evaluator of a programme to improve health literacy for vulnerable populations, in response to the COVID-19 pandemic. The Center for the Prevention of Health Disparities also offers field trips in ecology, along with health and wellness programmes for students in the community. The centre also runs the only pollen counting station accredited by the NAB in Northeast Florida. For Professor Seymour, and immunologists like him, work is not confined to the lab!
• You could work for a university or in industry, working on advancing treatments and working towards health equity.
• Find an internship during the summer of your undergraduate degree – most universities will offer an internship programme.
• The American Public Health Association provides information on internships for undergraduate and graduate students.
• The American Association of Immunologists (AAI) has a careers page on its website.
• The British Immunology Society hosts a wealth of information about careers in the field.
• The UK’s National Health Service (NHS) also provides useful information.
• Study chemistry, biology and mathematics at high school.
• At university, study chemistry, microbiology or cell biology.
• With the growing importance of bioinformatics and data, Professor Seymour recommends studying computing and data science when given the opportunity.
• Gain experience with first-hand immunology through an internship or work experience programme.
• Study for a PhD in immunology or become a physician and specialise in allergy, immunology or pulmonology. Information on PhDs in immunology can be found here.
HOW DID YOUR CHILDHOOD INFLUENCE YOUR CAREER PATH?
As a child growing up in a farming community on the coast of South America in the country of Guyana, I experienced severe episodes of hives, particularly during the harvest season. My grandmother used many home remedies for its treatment. Being an inquisitive child, my curiosity as to why these hives only occurred at a specific time of the year followed me into my college years. I was relieved when I realised that there was an explanation for the problem that had affected me in my childhood. Learning about the role my immune system played in my childhood ailments sparked my interest and motivated me to learn more.
HOW DO YOU OVERCOME OBSTACLES IN YOUR WORK?
There are always going to be obstacles in life. We must expect them, confront them and be able to adjust when they occur. However, with perseverance and the ability to learn from our mistakes and the mistakes of others, we can overcome most obstacles. Switching off from work can be easy at times, especially when my family requires attention! Vacations are a must; you need to be able to learn how to relax. Sometimes, it’s in those moments that your greatest inspirations are acquired.
WHAT ARE YOUR PROUDEST CAREER ACHIEVEMENTS, SO FAR?
I have worked with Dr Robert L. Coffman, at the DNAX Research Institute, who discovered that there were multiple types of T helper cells by looking at the cytokines the cells secrete during an immune response. We were the first to demonstrate, in an animal model of lung inflammation, that antibodies against IL5 (a cytokine secreted by Th2 cells) will inhibit lung inflammation caused by eosinophils (a type of white blood cell)*. I am gratified to know that studies like this have paved the way for the development of new drugs that treat conditions in patients such as eosinophilic asthma. I am also proud to know that my definitive studies on ETS with Dr Laurel Gershwin of the TRDRP at UCD played a role in changing public policy in California and the world**. I am also proud that I established the only pollen counting station accredited by the NAB in Northeast Florida. It is one of only three such stations in the state. However, my proudest moments will continue to be when I see the undergraduate students whom I have mentored moving on into graduate, pharmacy and medical schools.
*Antibody to interleukin-5 inhibits Helminth-induced eosinophilia in mice. (1989). Coffman, R.L., Seymour, B.W.P. Hudak, S., Jackson, J. and Rennick, D. Science 245: 308-310.
**Second-hand smoke is an adjuvant for T helper 2 responses in a murine model of allergy (1997). Seymour, B.W.P., Pinkerton, K.E., Friebertshauser, K, Coffman, R.L. and Gershwin, L.J. J. Immunol. 159: 6169-6175.
01 Take part in internships during your undergraduate studies to get first-hand experience of many areas of biology and to meet researchers.
02 Some institutions offer post-baccalaureate programmes, which are paid placements that prepare you for graduate education. If you can, get involved in them.
03 Study computing and data science to future-proof your career.
04 Be willing to work hard and be dedicated to science.
Write it in the comments box below and Professor Seymour will get back to you. (Remember, researchers are very busy people, so you may have to wait a few days.)