What happens when our blood production system fails?
A healthy adult produces billions of new blood cells every single day. Yet for some people, the process that generates these cells does not function properly, potentially resulting in blood cancer. At the Albert Einstein College of Medicine in New York, USA, Dr Kristina Ames has been investigating why blood production problems occur and has discovered a potential treatment that could restore the function of blood production cells.
TALK LIKE A CELL BIOLOGIST
Acute myeloid leukaemia (AML) — a form of blood cancer
AKT — a protein that regulates a wide variety of cellular functions including cell growth, division and survival
Autophagosomes — the vesicles used in autophagy
Autophagy — the process of cellular recycling and cleaning of unnecessary cellular components, such as non-functional organelles and proteins
Blast — an abnormal immature white blood cell that multiplies uncontrollably, filling up the bone marrow and preventing the production of other blood cells
Differentiation — the ability of a cell to become a cell of a different type
Haematopoiesis — the production of blood cells
Haematopoietic stem cells (HSCs) — cells found in bone marrow from which all blood cells are produced
Isoforms — functionally similar proteins with similar but not identical sequences of amino acids, encoded by different genes or by the same gene of different RNA transcripts
Mouse model — a genetically engineered lab mouse used to study human disease
Myelodysplastic syndrome (MDS) — a form of blood cancer
Phosphoinositide 3 kinase (PI3K) — the family of signal transducer enzymes involved in cellular functions, such as cell growth, proliferation, differentiation, motility, survival and intracellular trafficking
PI3K/AKT — a signalling pathway that regulates a wide variety of cellular functions including cell survival and growth (where PI3K enzymes and AKT protein are the main regulators)
Progenitor cells — cells produced from HSCs that have not fully differentiated into mature blood cells
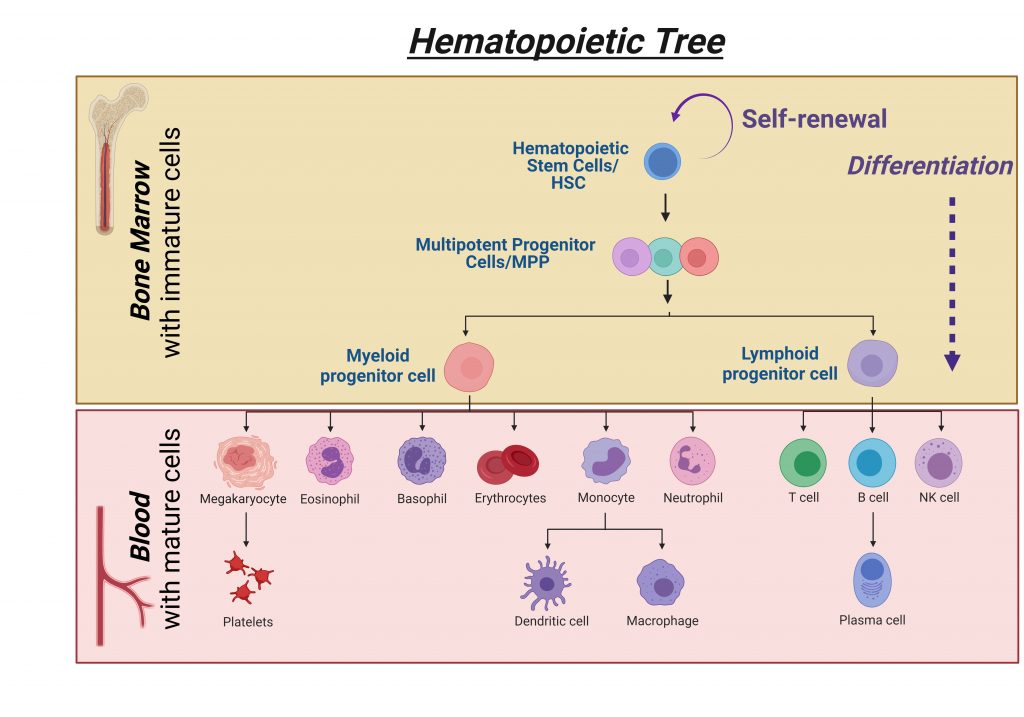
Have you ever considered what the blood pumping around your body contains? It is a complex mixture of living cells that each have their own important role to play. Red blood cells carry gases around the body, delivering oxygen to every cell and removing carbon dioxide. Platelets cause your blood to clot when you cut yourself, so that the bleeding stops. Granulocytes help the body fight bacterial infections, while macrophages digest microorganisms and remove dead cells. B cells produce antibodies that attack invading viruses, and T cells destroy infected cells in the body.
An adult human body contains approximately 4.5-5.7 litres of blood, which makes up about 10% of the body’s weight. But how does the body create the trillions of cells needed to maintain this volume of blood? And what happens when this process goes wrong?
How are blood cells produced?
“The process of blood cell production is called haematopoiesis,” says Dr Kristina Ames, a cell biologist at the Albert Einstein College of Medicine. “In a healthy adult, approximately 1011-1012 new blood cells are produced every day!” This monumental daily creation of new blood (including approximately 2 million new red blood cells every second) is essential for maintaining a healthy blood system.
Haematopoiesis occurs from haematopoietic stem cells (HSCs) which exist in the marrow within your bones. These HSCs can self-renew, meaning they can generate more of themselves, so the supply never runs out. HSCs can also differentiate, meaning they can turn into progenitor cells, which then turn into all the other types of blood cell, such as macrophages, platelets and T cells. Once the blood cells produced by HSCs are mature, they move out of the bone marrow and into the blood system, where they circulate around the body in the bloodstream, fulfilling their required role.
What happens when haematopoiesis goes wrong?
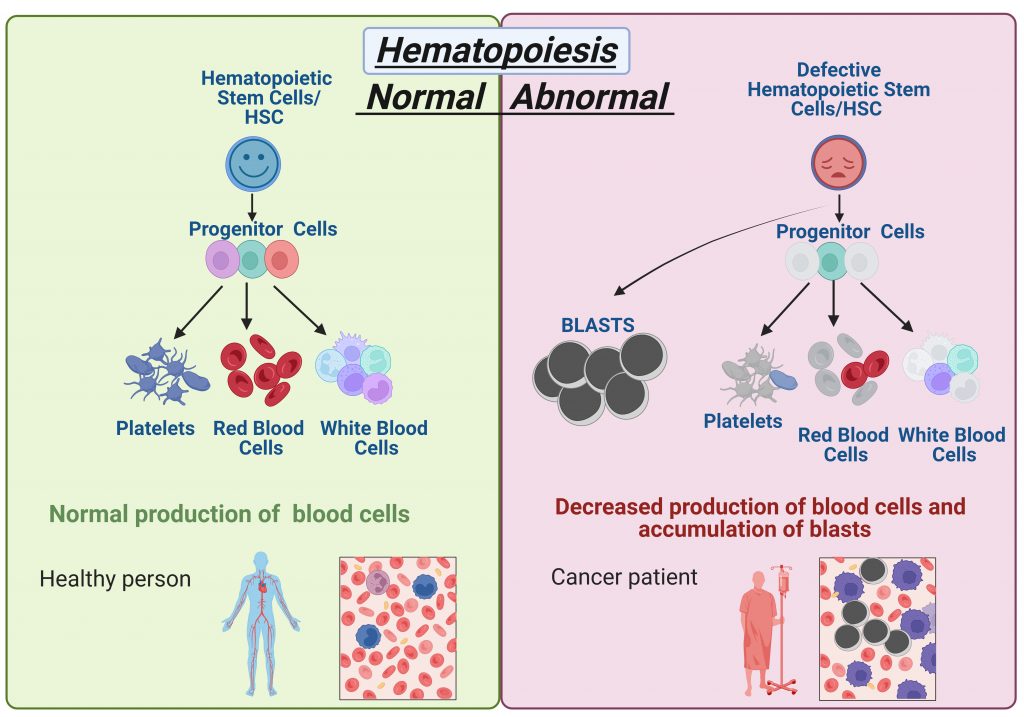
To generate new blood cells correctly, there must be a balance between HSC self-renewal and differentiation. If this balance is disturbed and the differentiation process is abnormal, improperly undifferentiated blood cells will remain in their altered immature form, known as ‘blasts’, which can lead to cancer.
Myelodysplastic syndrome (MDS) is a type of cancer that occurs when HSCs do not differentiate into mature blood cells, resulting in an increased number of stem cells and the presence of blasts in the bloodstream. If too many blasts are formed, MDS can develop into acute myeloid leukaemia (AML). About 20,000 people are diagnosed with MDS every year in the US, and up to 40% of MDS patients progress to AML. Most patients diagnosed with AML will die within two years.
“The causes of MDS and its progression into AML are poorly understood, so research into the initiation of these diseases is needed to inform better treatment options for patients,” says Kristina.
What signals control haematopoiesis?
To maintain proper haematopoiesis, molecules in the body, such as growth factors, send signals to HSCs in the bone marrow to inform them about conditions in the body and whether they need to produce new blood cells. “One of the most important signalling pathways that conveys resource availability is the phosphoinositide 3-kinase PI3K/AKT pathway,” says Kristina. “These enzymes receive signals from the growth factors that activate the AKT pathway, which in turn relays information about resource availability for the multiple downstream effectors that regulate vital cell processes, such as metabolism, glucose balance, cell proliferation and cell death.” The specific PI3K/AKT signalling pathway is therefore essential for regulating the cellular processes.
What is Kristina investigating?
“Our lab is specifically interested in the role of the PI3K/AKT signalling pathway in haematopoiesis,” says Kristina. The PI3K/AKT signalling pathway is activated during several types of cancer, so blocking this pathway is a therapeutic technique for cancer treatment. PI3K inhibitors are commonly used to treat cancer patients, but the role of PI3K in regulating HSC function is still poorly understood. If Kristina can determine this, it could lead to improved blood cancer treatments.
The PI3K pathway regulates the cellular processes for multiple tissues in an organism, but Kristina only wants to study its influence on HSCs and progenitor cells. To do that, she had to create a novel mouse model that allows her to investigate the effects of PI3K in the haematopoietic tissue she is interested in. “We made a unique Triple Knock Out (TKO) model that allows us to delete the three redundant isoforms of PI3K in an adult mouse haematopoietic system without affecting the development of the mouse,” Kristina explains. “Thus, we can access the role of the PI3Ks in adult haematopoiesis.”
What has Kristina discovered?
Kristina used her mouse model to investigate whether TKO mice had normal blood production. She discovered that when the three isoforms of PI3K were removed from a mouse, it led to a significant decrease in the populations of all types of blood cells. This is a condition known as pancytopenia and suggests that the HSCs in the TKO mouse models were defective.
To test if this was the case, Kristina performed bone marrow transplants on the TKO mice. “Usually, bone marrow has a small population of HSCs that is very efficient in self-renewal and differentiation,” explains Kristina. “But in our TKO mice models, we found that despite a decrease in the total number of blood cells, there was an increase in the number of HSCs. However, this high count of HSCs did not result in a high number of progenitor cells, suggesting a differentiation problem in TKO HSCs.”
Reference
https://doi.org/10.33424/FUTURUM411
Kristina then examined the bone marrow cells in her TKO mice. “The bone marrow cells of TKO mice showed signs of abnormal differentiation, which are very similar to those seen in patients with MDS,” she says. “We found that TKO mice share multiple features with patients who were diagnosed with MDS, including increased self-renewal of stem cells, decreased differentiation and the presence of blasts.” Some TKO mice even began to progress to a more serious condition, in the same way some patients with MDS progress to AML.
To determine the mechanism that causes the changes in HSCs and progenitor cells when PI3K isoforms are lost, Kristina took advantage of next-generation sequencing techniques. She discovered that in TKO mice, HSCs are unable to regulate the process of autophagy, in which cells recycle unnecessary organelles and clean themselves. In autophagy, vesicles known as autophagosomes degrade and recycle non-functional organelles and proteins for further cellular use, thereby keeping the cell clean and healthy. However, mice without PI3K isoforms displayed decreased expression of several autophagy genes, leading to a compromised recycling process within the cell and an accumulation of autophagosomes with undegraded cellular debris. “Intriguingly, we also found an accumulation of autophagosomes in human pre-MDS stem cells,” says Kristina.
How will Kristina’s research help people with cancer?
Kristina’s research has shown that a lack of PI3K signalling disrupts autophagy in HSCs, and that this causes defective differentiation. From these discoveries, she hypothesised that if autophagy could be activated with drugs, it would improve differentiation of HSCs in bone marrow. “And that is exactly what we found!” she says. “Treatment of stem cells that have compromised PI3K signalling with autophagy-inducing drugs improved cellular recycling and, as a result, improved the differentiation of HSCs.” Kristina concludes that impaired autophagy is a key mechanism for disrupted HSC differentiation in patients with MDS, and that autophagy-inducing drugs could help to restore HSC function. Kristina’s mouse model research is, therefore, essential for understanding the causes of and testing treatments for blood cancers, which will result in improved outcomes for people with MDS and AML blood cancers.
 Dr Kristina Ames
Dr Kristina Ames
Cell Biology Department, Stem Cell Institute, Albert Einstein College of Medicine, New York, USA
Field of research: Cell Biology
Research project: Investigating the role of the PI3K/AKT signalling pathway in the production of blood cells
Funders: US National Institutes of Health (NIH), National Cancer Institute, National Heart, Lung and Blood Institute
ABOUT CELL BIOLOGY
Cell biology is the branch of biology that studies organisms at the cellular level. Cells are the functional unit of life and, traditionally, cell biologists focused on studying individual cells or genes to understand their function. However, scientists know that cells and the molecules within them do not act in isolation, so it is important to study cells within the wider context of the whole organism. “I enjoy asking big questions from the perspective of the whole organism,” says Kristina. “This allows me to see the consequences of cell modifications in the whole organism, not just in individual cells. Every small change we introduce at the cellular level can lead to great consequences at the organismal level.”
What do cell biologists do?
Cell biologists spend a lot of time in the lab conducting experiments. “We use signal-based methods where scientists control cells and their functions by making changes to the expression of specific target genes. We monitor these introduced chances using various techniques, such as microscopy, flow cytometry, protein blotting and multiple molecular assays, that, together, allow us to understand protein interactions and gene function,” says Kristina. “The field is rapidly developing, so nowadays we can combine these techniques with big dataset processing and next-generation sequencing.” These new approaches have broadened cellular and molecular biology research. Kristina explains, “These advances give the exciting opportunity to combine ‘wet lab’ (lab-based experiments) and ‘dry-lab’ (computer-based analyses) approaches that have the potential to result in more precise experimental design and subsequent studies.”
As a cell biologist, you may find yourself growing cell cultures, working with microscopes, sequencing DNA, examining the cellular structures and functions of organelles and proteins, or investigating cellular mechanisms.
How could you advance our knowledge of cells and contribute to this exciting field?
Pathway from school to cell biology
• At school and post-16, study biology alongside other science and maths classes. “All science classes will be beneficial for working in a cell biology lab,” says Kristina.
• Kristina also recommends learning computer science and coding, as these skills are becoming very useful for cell biologists.
• Some universities offer degrees specifically in cell biology. Otherwise, degrees in biology, molecular biology or biochemistry could lead to a career in cell biology.
• “What I like about science is that it’s not rigid,” says Kristina. “You can take classes in the subjects that appeal to you and go in the direction that interests you. If you like something, go for it!”
Explore careers in cell biology
• Many cell biologists, such as Kristina, apply their skills in the medical field, enabling their research to lead to improvements in human health. Others focus on plant or animal cell research, to improve the health of plants and animals.
• Kristina recommends looking for opportunities to participate in summer research programmes and internships to gain experience of working in a cell biology lab.
• The Albert Einstein College of Medicine has a summer research programme for high school students.
• Kristina helped establish BEYOND ALBERT (Bronx Einstein Youth Oncology Network Dedicated to Academic Learning, Biomedical Education and Research Training), a summer programme that allows high school students in the Bronx to undertake lab-based biology research projects.
• Zippia provides information about careers in cell biology, including the skills and qualifications you need and the salary you can expect.
Meet Kristina
I have always been interested in how things work and want to understand the details of everything around me. Early on, I discovered there are different ways to learn. You can get information from someone else, by reading or listening, or you can figure out the information for yourself. It was an amazing experience when I realised I could learn and discover by doing, but it’s even more exciting when I get my turn to tell the story! I became a scientist so I can find new things and tell other people about them.
The eureka moments are what make science so fascinating and rewarding. But science has also taught me to be patient. A lot of the time, everything moves very slowly. Answers are missing or findings don’t fit into the bigger picture. At that point, you need to trust the process. Keep adding the little pieces to your puzzle and, eventually, everything will connect. Savour the victory when it does!
I ask three questions along every step of my research: What? How? And why? WHAT is the exact question I am interested in at this moment? HOW will I answer it? WHY it is important? And WHAT other doors will these answers open? These questions guide me in science and in all aspects of my life.
The worst advice I was ever given was to multitask and balance things. I am the worst multitasker, I can’t balance and trying to follow this advice was very unproductive for me. Instead, I realised I am a ‘juggler’. I choose three tasks that need doing and focus on one at a time, rotating between each of them several times until they are finished. I don’t start anything new until one of the tasks is finished, because I become overwhelmed if I have to juggle more than three balls at once.
Any obstacle can be viewed from multiple perspectives. When you hit an obstacle, pause and look at it from a different perspective. You will often find the solution that is right in front of you!
I am enthusiastic about raising the next generation of biomedical professionals and am proud to have launched two educational programmes from the Montefiore Einstein Cancer Center. In one, high school students explore research methodologies, learn about experimental design and conduct their own research project. In the other, master’s students from the nearby Lehman College complete their thesis research at Montefiore Einstein Cancer Center, allowing them to become fully immersed in a research environment. I really enjoy bringing together science and education as I develop and define the vision, goals and strategies for research education programmes.
I love walking to decompress from daily stress. If I need to switch off for longer, I prefer to spend time in nature – I enjoy hiking and scuba diving. My favourite vacations are when I can dive with purpose and contribute to the citizen science of the GalapagosWhale Shark Project.
Kristina’s top tips
1. Always stay curious and keep asking questions.
2. Believe you can find your way to your destination by simply taking one little step at a time.
3. Keep moving. Take breaks when you need to, but never stop.
Do you have a question for Kristina?
Write it in the comments box below and Kristina will get back to you. (Remember, researchers are very busy people, so you may have to wait a few days.)