How can community voices transform HIV modelling and prevention?
In Kenya, men who have sex with men (MSM) face higher risks of HIV, yet their voices are often missing from the science that shapes health decisions. A team of academic and community researchers, including Professor Sharmistha Mishra, Jeffrey Walimbwa, Nancy Tahmo and Dr Lisa Lazarus, is co-developing mathematical models of HIV with MSM organisations. By combining lived experiences with mathematical models and epidemiology, this community-led project aims to create more accurate models, improve HIV prevention and empower communities.
Talk like an epidemiologist and social scientist
Ethnography — a research method used to explore social and cultural practices and contexts, which involves spending time with communities, building relationships and collecting data (through conversations, observations and note taking) to build an understanding of social worlds
Epidemic — a widespread disease outbreak
HIV (human immunodeficiency virus) — a virus (passed between people through unprotected sex or blood) that weakens the immune system, leaving someone vulnerable to other infections. Medicines can prevent HIV spreading and supress it in people living with HIV
Mathematical model — a set of equations and data that represents mechanisms in a real system, commonly used in epidemiology to study how and why infections spread
Mechanism — a pathway that links events or experiences, such as how people are connected to each other (our social network is a type of mechanism) or how one infection could lead to many infections in a short period of time
Participatory modelling — co-creating mathematical models with affected community members to ensure data and assumptions about mechanisms match real-life experiences and improve the usefulness of the results
Prevalence — the percentage of people in a population who have an infection or disease at a specific time
Public health intervention — an organised action (e.g., testing, vaccines, treatment or education) designed to prevent infection and improve health in a whole community, not just in one person
HIV (human immunodeficiency virus) is a virus that, if untreated, weakens the body’s immune system and can lead to AIDS (acquired immunodeficiency syndrome). Although there is currently no cure for HIV, there are medicines that can completely supress the virus and keep the immune system strong and healthy. There are also medicines that prevent the virus from being passed on and medicines that prevent people from acquiring HIV. Without these medicines, the virus can be spread through unprotected sex or blood-to-blood contact.
With the right medicines and prevention tools, HIV transmission can be reduced to zero. Yet access to prevention and care is not equal everywhere. In Kenya, around 1.4 million adults are living with HIV. And, like in many places, the Kenyan HIV epidemic has disproportionately affected men who have sex with men (MSM). “HIV prevalence among MSM is around 19%,” says Jeffrey Walimbwa, Program Manager for Ishtar MSM, a community organisation that provides HIV testing, treatment, counselling and legal support for MSM in Nairobi. This is nearly three times higher than in the wider population. These numbers reflect social realities rather than biological differences. “Criminalisation and discrimination of same-sex partnerships and stigma related to sex and HIV are large barriers to accessing the services and medicines that can help prevent and treat HIV,” explains Professor Sharmistha Mishra, an infectious diseases doctor and epidemiologist at the University of Toronto in Canada.
“There are limited MSM-friendly services that provide HIV treatment and prevention in Kenya,” explains Jeffrey. “Criminalisation of same-sex relationships means people are scared to seek help due to fear of arrest. Most of the interventions are led by community drop-in centres started by MSM.”
By combining academic expertise with MSM community organisations, Sharmistha and Jeffrey are co-developing mathematical models of the HIV epidemic with affected communities.
What are mathematical models of epidemics?
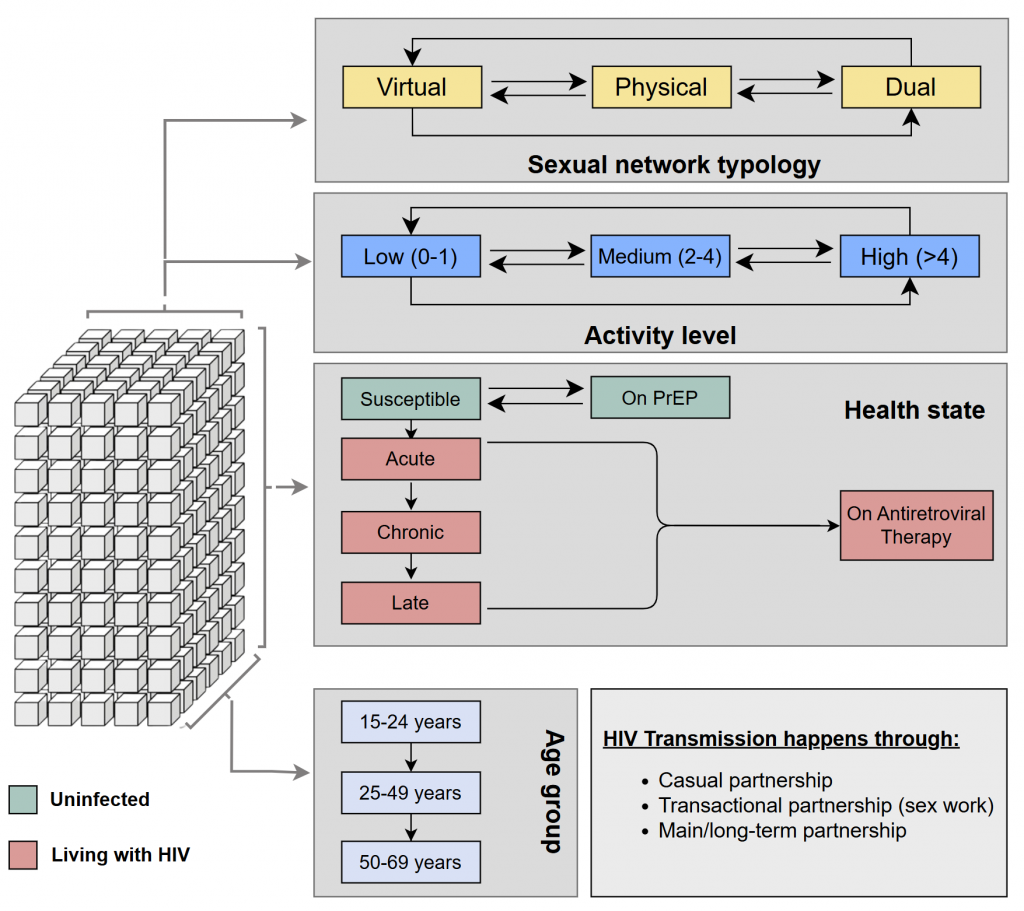
Mathematical models help scientists understand how viruses spread through populations. First, researchers design the ‘architecture’ of the model by mathematically describing important mechanisms, such as how a virus behaves in the body and how people come into contact with each other such that a virus could be passed on (transmission). There are different ways in which people come into contact and different reasons for contacts, so depending on the virus being studied, what is meant by a ‘contact’ can be different. For example, for HIV, contacts often refer to sexual intercourse.
Modellers and epidemiologists then add data to the model, such as infection rates or the number of people diagnosed with the infection over time, to test whether the model reflects what is observed to be happening in real life. Once a model is working well, it can be used to test ‘what if?’ questions to explore the effects of different public health intervention strategies designed to reduce the spread of infection.
Public health authorities can use these models to predict how epidemics may spread, plan how resources should be allocated and decide which prevention strategies are likely to work best. “For example, government public health teams widely used mathematical models during the COVID-19 pandemic,” says Sharmistha. They are also used by community organisations who are managing outbreaks, and for advocacy teams to decide what resources are needed and what programmes to prioritise.
How are communities shaping mathematical models of HIV?
This project is rooted in community leadership, meaning that team members bring direct or indirect lived experiences of HIV, knowledge of community needs and practical understanding from working in HIV programmes. “This project began when Jeffrey approached me and said Ishtar MSM wanted to develop mathematical modelling projects to understand the spread of HIV,” says Sharmistha. “Input from MSM shapes the epidemiology models we are building because, instead of models relying on assumptions from literature and academia, they are based on real lived experiences and knowledge from community members.”
“At the same time, community researchers are learning how mathematical models are built and how their results can influence HIV services and policy decisions,” says Nancy Tahmo, an epidemiology PhD student at the University of Toronto. This growing understanding helps communities engage more confidently with science and advocate for better care.
Why is participatory modelling so important?
“Epidemiology models are used to inform public health interventions and decisions, so it is essential that the people whose lives are impacted by these decisions have ownership over the modelling process,” explains Sharmistha. By involving community members directly, the project replaces assumptions with real lived experiences, improving the accuracy and relevance of the models. It also gives communities more knowledge, and therefore more power, to make decisions about their own health, which is especially important for groups who have historically been marginalised.
The project also includes an ethnography to capture the research process. “Our ethnography involves taking detailed ‘field notes’ to help us document and analyse our participatory processes to better understand the ethical implications of our work,” says Dr Lisa Lazarus, a social scientist at the University of Manitoba in Canada. “This allows us to share lessons from our collaboration with others who might be interested in starting their own participatory modelling projects.”
For community partners, the benefits of participatory modelling go far beyond science. “This project has empowered community members with skills to unpack data into language they can understand,” says Jeffrey. Through project training workshops, community members learnt how to clean data, address data quality issues, write computer code and formulate research questions. “With these skills, we have gone back to our organisations to work on our data, and now our outlook has taken a different form,” says Jeffrey. “We feel empowered to understand data in a professional way and we call ourselves ‘community professors’ with the knowledge and skills we have learnt.”
What has the project achieved so far?
Reference
https://doi.org/10.33424/FUTURUM681
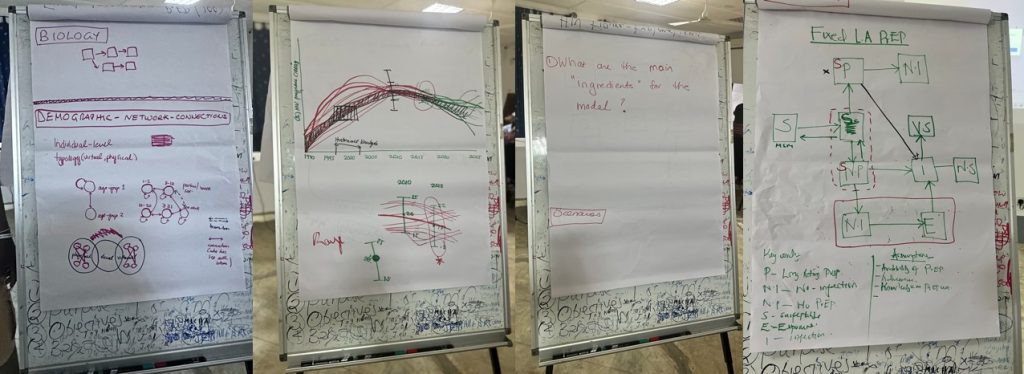
Over the past two years, the team has run a series of workshops with community members, starting by teaching the basics of data systems, modelling concepts and terminology. These workshops gradually built up to a stage where the community members co-designed their own mathematical model alongside the academic researchers. “This was a great success – it took a lot of knowledge sharing and training together to get to this point,” says Sharmistha. “The fact that community members co-designed the architecture of the mathematical model means it is based on their real lived experiences instead of just assumptions from the academic literature.”
Another key achievement has been training community members to lead the analysis of data collected by local MSM organisations. “These data become the inputs for our co-developed mathematical models to better understand the persistence of HIV epidemics,” explains Sharmistha.
An important component of the project involved critically reviewing over 9,000 published infectious disease models to examine how often community participation is included. Several community members were involved in the review process. “Preliminary results confirm our hypothesis that community involvement in mathematical modelling of infectious diseases is still quite rare,” says Nancy. “These insights reinforce the importance of our work – by co-developing a model with community partners, we are contributing to the evidence that participatory modelling can uniquely foster representation and the relevance of research.”
Lastly, during the model co-development process, the team recognised that meaningful community participation requires a shared understanding of modelling fundamentals. To support this, they developed a digital learning module that explains key modelling concepts and provides examples relevant to the local context. One of the community researchers helped refine the module before it was shared with the group, ensuring it was practical and accessible. These steps have strengthened both the skills and confidence of community researchers, enabling them to contribute to the models, interpret data effectively, and apply findings to HIV prevention and care in their communities.
“When community voices drive modelling, results are richer and more impactful for advocacy and designing interventions,” says Jeffrey. “This participatory modelling process proves that community expertise is essential, and it challenges traditional assumptions about who can contribute to scientific understanding.”
Research project: Co-developing mathematical models of HIV epidemics with affected communities
Fields of research: Mathematical modelling; epidemiology; social sciences
Funder: New Frontiers in Research Fund (NFRF) – Exploration grant number NFRFE-2023-00436
About the intersection of infectious disease epidemiology and social sciences
Epidemiology is the study of how infections spread through populations and how they can be prevented or controlled. “Epidemiologists try to understand patterns of infection, which could be at a community or whole population level,” says Sharmistha. “By understanding how an infectious disease might spread, epidemiologists try to understand how we can support communities and populations to prevent the spread and become healthier.”
When combined with insights from social sciences, epidemiology gains a deeper understanding of human behaviour, community dynamics and the structural factors that shape health outcomes. “Critical social scientists are interested in better understanding issues of power, relationships, and social and political contexts,” says Lisa. “The ethnographic methods that we have added to our project aim to track ethical issues in attempts to make visible what is often hidden in projects.” This interdisciplinary approach ensures that models and public health interventions are grounded not only in biological and statistical data but also in lived experiences and community knowledge.
One of the most rewarding aspects of this work is seeing how diverse perspectives come together to tackle complex health challenges. Community members bring insights that can reshape scientific thinking, prompting new questions, simulations or analyses that would not have arisen otherwise. “Communities know their needs better than researchers can ever imagine, and they are eager and motivated to see the research contribute to something positive,” says Nancy. For researchers, these interactions, which are often informal conversations, highlight the importance of integrating community knowledge with epidemiological methods, ensuring that models and interventions are both scientifically robust and truly responsive to the communities they serve. Witnessing community members gain skills and ownership in the research process is also deeply rewarding, as it demonstrates how participatory approaches can democratise science and amplify the voices of those most affected by health decisions.
Pathway from school to epidemiology and social sciences
Epidemiology, mathematical modelling and the social sciences are very broad and interdisciplinary, so almost any educational path could lead you to a career in these fields!
In high school, focus on mathematics, biology, computing, social studies and humanities.
At university, it would be useful to take courses in epidemiology, public health, social sciences, sociology, anthropology or health policy.
“Epidemiologists and social scientists need critical thinking skills to question what they observe and critically analyse data, as well as communication skills to explain results,” says Sharmistha. “Epidemiologists also need to be able to think logically and creatively to solve problems – board games and escape rooms are great for developing these skills!”
“Social scientists often work with social theories (which involves a lot of reading) and analyse qualitative data,” says Lisa. “Writing skills are also incredibly important.”
Explore careers in epidemiology and social sciences
“Epidemiologists critically examine data and try to explain what is going on – skills which can be applied in a wide range of areas from public health to wildlife ecology to genetics to virology,” explains Sharmistha. “Social epidemiologists use epidemiology principles and tools to understand and address inequalities, not just in health but in any sector of society.”
“Social sciences is not a single field, so there are endless career possibilities, depending on your interests,” says Lisa.
“If you’re interested in epidemiology or modelling, remember that numbers only make sense in context,” says Nancy. “Take every opportunity to connect with communities, because understanding the realities behind the data will make you a far stronger scientist.”
“Volunteer with community-based organisations to build relationships and learn about community needs,” advises Lisa. “Come in ready to listen to what people are telling you about their own needs, and partner in ways that support community-identified approaches.”
Many international organisations provide learning resources, training opportunities and insights into careers in epidemiology and social sciences, such as the World Health Organization (who.int) and UNAIDS (unaids.org).
Meet Sharmistha
 Professor and Infectious Diseases Doctor, Department of Medicine, University of Toronto, Canada
Professor and Infectious Diseases Doctor, Department of Medicine, University of Toronto, Canada
As a child, my family moved from India to Canada. We moved in December and my first memory is of huge mounds of snow and sliding down snowy hills in the park! I remember missing my extended family back home a lot, but over time, I found a community of new friends. Initially, I was the ‘odd kid out’ at my new school in Canada as there were only two other non-white students. Over the years, more children from different backgrounds gradually arrived which made a difference as we gravitated toward each other.
As a teenager, I think medicine appealed to me because it was what many of my friends were interested in. It wasn’t until my third year of medical school, when I first got a chance to practice it, that I realised I loved medicine. I had no plans to do research until the very end of my clinical training, when I attended a talk about the collaborative response to the HIV epidemic in India. This inspired my interest in epidemiology.
As an infectious diseases doctor, I spend my days seeing patients, listening to their stories, and trying to diagnose and treat their conditions. As a mathematical modeller and epidemiologist, a typical day involves problem-solving by drawing diagrams of mechanisms and writing or debugging code to run epidemiology models.
Co-developing mathematical models with affected communities is very rewarding. I like it when something unexpected arrives from community expertise to re-shape our thinking.
I worked with the World Health Organization during the 2014 Ebola epidemic in Sierra Leone. I used my clinical expertise as an infectious disease doctor to care for sick patients, and I used my epidemiology expertise to support outbreak investigation and management. I collaborated with colleagues in Sierra Leone to study the impacts of the Ebola outbreak on other health conditions and services.
Sharmistha’s top tips
1. I think 15-year-old you could be very surprised by what 25-year-old or 35-year-old you ends up doing with your life and work!
2. Looking back, the most fulfilling work experiences were the ones that I was most scared of trying.
Meet Jeffrey
 Program Manager, Ishtar MSM, Kenya; Research Lead, Community Research and Technical Support Hub
Program Manager, Ishtar MSM, Kenya; Research Lead, Community Research and Technical Support Hub
When I was a teenager, I dreamt of becoming a chef. Cooking was my creative outlet, and it taught me patience and attention to detail. I also enjoyed dancing, which was another way for me to express myself and connect with others, and reading, which opened my mind to new ideas and different worlds.
My first experience with research came during a fellowship at the Human Rights Advocacy Program at Columbia University, USA. At the time, I didn’t see myself as a ‘researcher’. I was an advocate, deeply committed to the rights and dignity of gay men. That fellowship opened my eyes to how research could be a powerful form of advocacy when grounded in the voices and experiences of the communities it aims to serve.
For me, research is never just about the data – it’s about the people behind the data. I’ve participated as a researcher in numerous studies, always grounded in the belief that data must lead to action.
I believe that communities are the experts in their own lives. For too long, research on gay men has been done to communities, not with them. To challenge this, I co-founded Action for Access, an international community-led study into gay men’s health and rights, to show that research can be a tool for empowerment when it is community led.
In my role at Ishtar MSM, I am involved in coordinating our programmes, advocating for community needs, engaging with policymakers, ensuring our interventions are impactful, and translating research into actionable tools that inform policy and practice. I have also established a Community Research and Technical Support Hub to strengthen community-led research projects.
I am passionate about community-based participatory research because it centres the voices and expertise of those affected by the issues being studied. It is empowering to see how co-developing mathematical models of HIV fosters a sense of ownership among MSM as they take an active role in shaping the models.
Jeffrey’s top tips
1. Stay consistent and focused.
2. It is not an easy road if you are gay in Kenya, where you can be at risk of violence. So stay strong.
Meet Nancy
 PhD student, Division of Epidemiology, University of Toronto, Canada
PhD student, Division of Epidemiology, University of Toronto, Canada
I have always wanted to bring hope to people, because I believe keeping hope alive helps people stay motivated and thrive. This led me toward community health, as I understood first-hand the vicious cycle of poor health and well-being.
I wanted to be a doctor, so I studied science subjects at school and took the medical entrance examination in Cameroon. But I failed. I studied biochemistry at university instead, where I found my true calling in infectious disease prevention and control. In hindsight, my interests have matured in a beautiful way because of that failure.
My inspiration to become an epidemiologist came from Dr Judith Shang at the Centers for Disease Control and Prevention in Cameroon. She was the first person to talk to me about public health. Until that day, I only knew about healthcare, but through her, I learned about the critical role of public health in supporting population-wide disease prevention and control efforts.
In the middle of the COVID-19 pandemic, I moved by myself to Omaha, Nebraska – a place that felt worlds apart from Cameroon. The culture, weather and pace of life were all very different. My biggest challenge was navigating imposter syndrome as a young Black African woman in a predominantly White Midwest environment. At the same time, the move was transformative, helping me learn more about myself and truly become independent.
During my work with zoonotic diseases (that spread from animals to humans) in Sub-Saharan Africa, I collaborated with research teams in Cameroon and the US to understand the burden of infectious diseases such as Ebola. We worked with tribal chiefs, communities and health district leaders to learn from their lived experiences, and we combined our findings from research and community conversations to inform surveillance and response efforts.
Nancy’s top tips
1. Remember to enjoy the growth process. My journey hasn’t always gone as planned, as things have evolved in unexpected ways. So it is important to have a plan but to also stay open to the magic of the moment.
2. Surround yourself with good people who understand your vision and will support you along the way.
Meet Lisa

Assistant Professor, Institute for Global Public Health, College of Community and Global Health, University of Manitoba, Canada
As a teenager, I really enjoyed music and went to a lot of concerts. One of my first jobs was at a music store selling CDs, well before streaming became the main way that we listen to music.
I started my professional career as a social worker at a hospital-based clinic in Montreal, working with people living with HIV. While I loved my job, I became interested in the recurring systemic issues within the healthcare system. This led me to pursue a master’s degree in public health, where I met Dr Robert Lorway and learnt about community-based research methodologies. Community-based research allows me to address systemic health issues while collaborating with community members who have lived experiences of interacting with healthcare systems. Rob and I still work together, and he is also a member of this participatory modelling project.
I credit Ashodaya Samithi with my on-the-ground education in community-led practices. Ashodaya Samithi is a sex worker-led organisation in India which was established in response to the HIV epidemic. Community leaders run the organisation, which provides medical care, prioritises community voices in health interventions, and advocates for the needs and rights of sex workers. I began collaborating with Ashodaya Samithi in 2009 and, for my doctoral research, I studied how the organisation’s community-led delivery of HIV prevention medicine among sex workers increased uptake.
There really is no ‘typical’ day as a social sciences researcher! When I am travelling for work, I spend time with community partners collaborating on our research activities. This includes meeting to co-develop our research methods, working together to analyse data, and discussing how to disseminate our findings to community or government partners. When I am at the University of Manitoba, I write papers to share our findings, write grant applications to get funding for projects, and read about the latest research.
Lisa’s top tips
1. There are lots of avenues in public health research, so reach out to people who do work that interests you.
2. Spend time volunteering to build genuine relationships and listen to what communities are telling you.
With special thanks to the HEKA participatory modelling team: Allan Ogalo, Anthony Noah, Byron Odhiambo, Charles Kyalo, Fortune Ligare, Gilbert Asuri, Jedidah Wanjiku, Kennedy Mwendwa, Kennedy Olango, Kennedy Ouma, Loice Nekesa, Pascal Macharia, Silvano Tabbu, Adrienne K. Chan, Stefan Baral, Robert Lorway, Nancy Tahmo, Jeffrey Walimbwa Wambaya, Lisa Lazarus and Sharmistha Mishra
Do you have a question for the team?
Write it in the comments box below and they will get back to you. (Remember, researchers are very busy people, so you may have to wait a few days.)

Discover how epidemiologists use mathematical models to keep our food safe:
futurumcareers.com/can-mathematics-keep-our-food-safe-to-eat









0 Comments